
Since before November 2022 there have been some issues going on with rising tumour markers.
My oncologist and myself had been monitoring them.
Then something happened, my oncologist went on leave for a year.
We had talks before he left about possibilities of a treatment change or other options.
It was something I really feared doing.
A pectoral node on my “good” breast side was causing a problem.
I had new scans in March and the new oncology team didn’t have a face to face review with me of my scan with me, they decided to ring me with a telephone consultation.
It was a 5 minute call with a registrar who went through small talk, how are you, how are the side effects etc etc. And then stated that all was ok on the scans and well I will order scans for another 3 months time and yes everything is ok.
I wondered how something could resolve itself, so I contacted the secretary and asked her to send my scans over. And there was still progression – it was only small and some millimetres of change but still it was highlighted in the report.
Annoyed, I sent an email off to confirm the fact that there was obvious progression on the scan and that my tumour markers were also rising therefore to me there was correlation between the two.
Meantime I took myself off into “finding solutions” mode and contacted Radiotherapy UK and two radiotherapists in relation to whether a pectoral node can be radio-therapied – yes it could. And a breast surgeon who I knew well, asking if it was possible to have my breast removed but the issue was I have lymphoedema in the left breast now – not a good idea to remove re healing due to the lymphedema.
I was called to a face to face meeting to assess the node and the Oncologist then agreed there was an issue with the pectoral node and agreed to having a consultation for radiotherapy. I was due to go on holiday in a few weeks’ time and advised her of the dates to avoid but hopefully I could get the appointment before I went on holiday. The Friday before we went away on the Sunday I had a call to say I could come in on the Tuesday. So that communication didn’t work. Therefore I had to wait until I came back from holiday.
On holiday I noticed 4 more small areas above the pectoral node that were like small grains of rice. They had been there maybe a couple of weeks but now quite unnoticeable. They hadn’t gone away. Then a few more days later a lump appeared under my left arm where the band on the bra goes. Then another couple of days there was an area under my breast which was lumpy and it had never been like that.
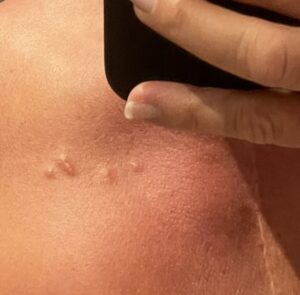
When I returned from holiday, my appointment to see the Radiologist was only 5 days later but of course but this wasn’t just about radiotherapy on the pectoral node, this was also about what the 3 areas are.
Upon examination he now needed biopsies of the areas and another scan before proceeding with whatever the plan was. So a few days later I was called to say there was an appointment at an new scanning centre in Oldham, at a cost of £10M it was there to reduce waiting times, reduce carbon emissions etc (don’t have to travel to The Christie or other centre) but they fell at the first hurdle with not even knowing what a port is and how to access this. Very, very long story short, I called around 2 other centres where I thought could access my port and was told no they couldn’t do it and go to Rochdale (I knew they wouldn’t do it there) and then told I’d have to go to the Christies (that defeats the object with a 2 hour round trip). So, as I know the Tameside Macmillan treatment unit and have treatment there every 3 weeks and do blood tests I booked myself in for a blood test (which was really port access) and turned up on the day explaining why I’d done this. They left the port access in and I went to the scan appointment. The receptionist at the scanning unit had told me to ring her when this was done so that they could tell the person scanning me but she had then left and I went through 4 more people talking about ports and access and it was dejavu again “we don’t do port access”. I turned up ½ hour later and was plonked into a very small cupboard of a side room with the same “we can’t access ports” well I’m here now and you can have a look. I finally got someone who knew what to do and they accessed the port and put the contrast through. Although, they came back in the room 4 times and the last time told me to move down the bed and when I went through the doughnut my feet banged on something at the bottom.
They flushed the port and then told me they couldn’t remove it. So, I had to keep the port in and sleep with it all night and go back to Tameside the next day to have the needle removed. Really not ideal for sleeping with OR reducing the carbon footprint, so I think that’s a fail.
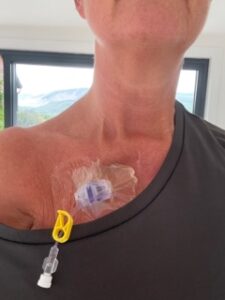
I had to have 3 biopsies at The Christie under local anaesthetic. It worried me that I was having these on my lymphoedema side so rang the breast nurse team and left a message. They came to see me when I was in the day unit at 1pm for the procedure and said the surgeon would discuss that. The nurse was great and supportive. As the surgeon would be working right under my left side and I asked for a screen up so I couldn’t see anything he was doing. I didn’t want him to be in my face doing surgery, cutting, pulling and tugging and then he also closed the wound by cauterization which they hadn’t advised and was a bit weird when I could feel something warm and hear the sizzle of flesh

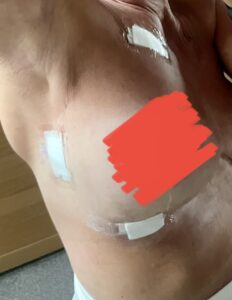
It all took around ½ hour and it was a busy surgery area, there must have been about 10 people in the area who were chatting quite loudly. A nurse was with me and talked to me and to tell me what they were doing but thankfully I couldn’t see it.
It was four hours in the hospital all together and we left at 5pm and headed back home. I had been given a leaflet and the surgeon came to see me after to discuss that I would need a wound check with a nurse a week later. They would send the letter to the GP but I needed to make an appointment. On the way home we called at the GP and asked if I could book into the nurse for a wound check. No sorry we don’t do that, but the district nurses do and she gave me a number to ring them in the morning as by this time it was nearly 6pm. The biopsies weren’t painful and I just took some paracetamol for any pain.
I rang the district nurse the next morning who also told me they don’t do wound checks. Who the hell does do wound checking? I rang Christies and told them the dilemma. I rang the GP and put a complaint in to them aswell as to the District nurses. The District nurses even had a referral by this time by email from the Christie to check me and they still wouldn’t do a wound check. Told me I was rude for complaining! Another problem that just makes all this more of a hassle than it should have been. You get weary sorting all the problems out.
Scans came back to confirm yet again that the pectoral node has grown slightly but no other areas. The biopsies confirmed that I am still HER2+ thankfully but ER/PR 0 so lost my receptors over the last 9.5 years. From the biopsies there was confirmed metastatic breast cancer in the skin (no it’s not skin cancer or melanoma). Bloody skin metastasis.
And to cut another long story short, I then had the option of Enhertu or Kadcyla and I’ve chosen Kadcyla as I may not get this 3rd line if NICE decide to remove this (which can happen) from 3rd line treatment which it is currently still an option.
It’s been a roller coaster of emotions, anger, sadness, upset, crying – having this disease is brutal and you go to bed at night and wake up the next day with the reality that hits you again that you have an incurable illness. I was back to the same time 9.5 years ago when I was rediagnosed with MBC and very upset. The feeling is just like when someone dies and for that split second on waking you forget what has happened and then reality hits. It happens every day.
I am though, in terms of living with metastatic breast cancer one of the lucky ones. I’ve lived for 9.5 years on perjeta and Herceptin/Phesgo and with additional surgeries and radiotherapies that have extended my life, at one point had no evidence of disease for just over 3.5 years. I wish everyone could have a “manageable” disease like I’ve had and not had the utter trauma and health emergencies that many of my friends have. I’m still alive and I still currently have options. I just hope that the treatment does work and I get a good response to the drug.
So here we go on treatment number 151/1 – I don’t like change but if it keeps me alive for longer then I’m all for it and I’ll never give up.
Oh and lastly I was very happy to see Danny who was a nurse at Tameside I’ve known for years at The Christie but left Tameside 3 years ago to work in a different area at The Christie in Withington. I saw him from afar and he turned around and ran to me! We hugged and it was lovely to see him. He made my day and I’m so pleased that I was there just to see him and catch up with each other. Hoping to see more of him in the future! Love you Danny x

