Firstly, I was overwhelmed by the lovely messages on twitter and Facebook from my blog post the day before I had surgery. And for the many cards and gifts I’ve had from friends. Thank you all so much x
The most amazing thing that also came out of sharing the blog was that I was contacted by two lovely ladies, one from twitter and one from Facebook that had had the same/similar surgery for secondary breast cancer in the sternum. One who had it 3 years ago and another who had it TEN years ago (and secondary in her lung which was also removed) and this lady is NED – get that NED!!!!! (to those of you who don’t know what that means it’s No Evidence of Disease – meaning remission) So this said to me that I was doing the right thing and I felt just slightly less nervous of the surgery..
From the pre op they give me 6 drinks to have – 4 the day before and 2 the morning of op 2 hours before surgery. So I did what I was told and then in the morning I woke at 6am to have the two drinks. I can taste them now yuk, they were carbohydrate drinks to keep my hydrated throughout the op and they tasted of lemon, sweet and slightly salty. Made me feel rather nauseous especially on an empty stomach. We dropped the children off at my friend Jayne’s house as Jeff was going to pick them up on the way back after agreeing it with school that they could both start late. I wanted them to be with their Dad after he had dropped me off.
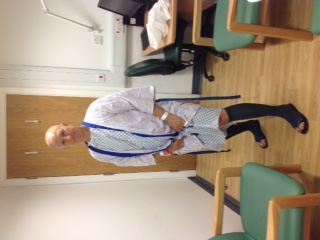
We parked and walked into the hospital towards the heart and lung unit. Handing my details into the reception for operations that day, we were shown to the seating area. It wasn’t long before a nurse collected us and I had various checks and notes written. Two bands put on each wrists with details and not to use the right arm due to my previous lymph node clearance. Then shown back out before going back into the room again and first my cardio thoracic surgeon Mr J came to see me and explain the procedure again, go through issues and shake my hand calmly but concerning to say he would see me later and that Jeff could come into see me that evening, he couldn’t see a problem with that. Then his colleague came to see me for consent forms. Mr O was lovely and again explained everything and I felt at ease. No airs or graces but yet I knew I was literally in safe hands. My Oncoplastic surgeon Mrs O’C came to see me and again explain the situation and to say she would see me later. Then two of the Anaesthetists came to see me, first T and then the loud Mr F ‘OH HELLO!’ he bellowed, a young willowy chap from Czech Republic (I think) who was very funny and the two of them were like a double act. So again questions and answers and consent forms and signatures. Everyone who I met was told by the nurse or previous staff “Jo has just cycled 62 miles on Sunday!” They couldn’t believe it…
Then our Scouse T (for those who don’t know what Scouse means it’s someone from Liverpool) decided to tell me a story about teeth as he questioned (after asking if I had any false teeth – no just a fixed bridge and 2 caps) we had this convoluted story for about 15 mins (to which at one point I thought the surgeon would be tapping his fingers wondering where we are) and then it felt like he was selling a dental service in Prague to me… it was pretty surreal to say the least! So they asked me to get changed into a gown and put some lovely paper knickers on and get some sexy surgical socks on and then T along with Jeff walked with me to the OR. Jeff was told he had to leave me and T told him the way out but not before we had an emotional hug and kiss with tears and then T said he’d look after me and with our arms around each other’s waists we walked together down the corridor, me crying in the room, where they helped me on the bed. Panic time. Hyperventilating and anxious they tried to get a line into my left arm without success then finally got one into my wrist and two of them were talking to me when another surgeon/anesthetist placed the mask on asked me to breathe and then I was gone and woke up what seemed like a second later. It was 7 hours later and two recovery staff were looking after me and I came round saying I didn’t feel well and my arms were dead from the elbow up and I couldn’t feel my chest or upper body. Feeling anxious about that and getting upset they said they would help and a surgeon came over to see me to check and they said they would reduce the epidural as it was making me feel like this. I could hear one of the staff talking to Jeff saying that I was out of the OR and awake and OK and that they were taking me up to the Critical Care Unit.
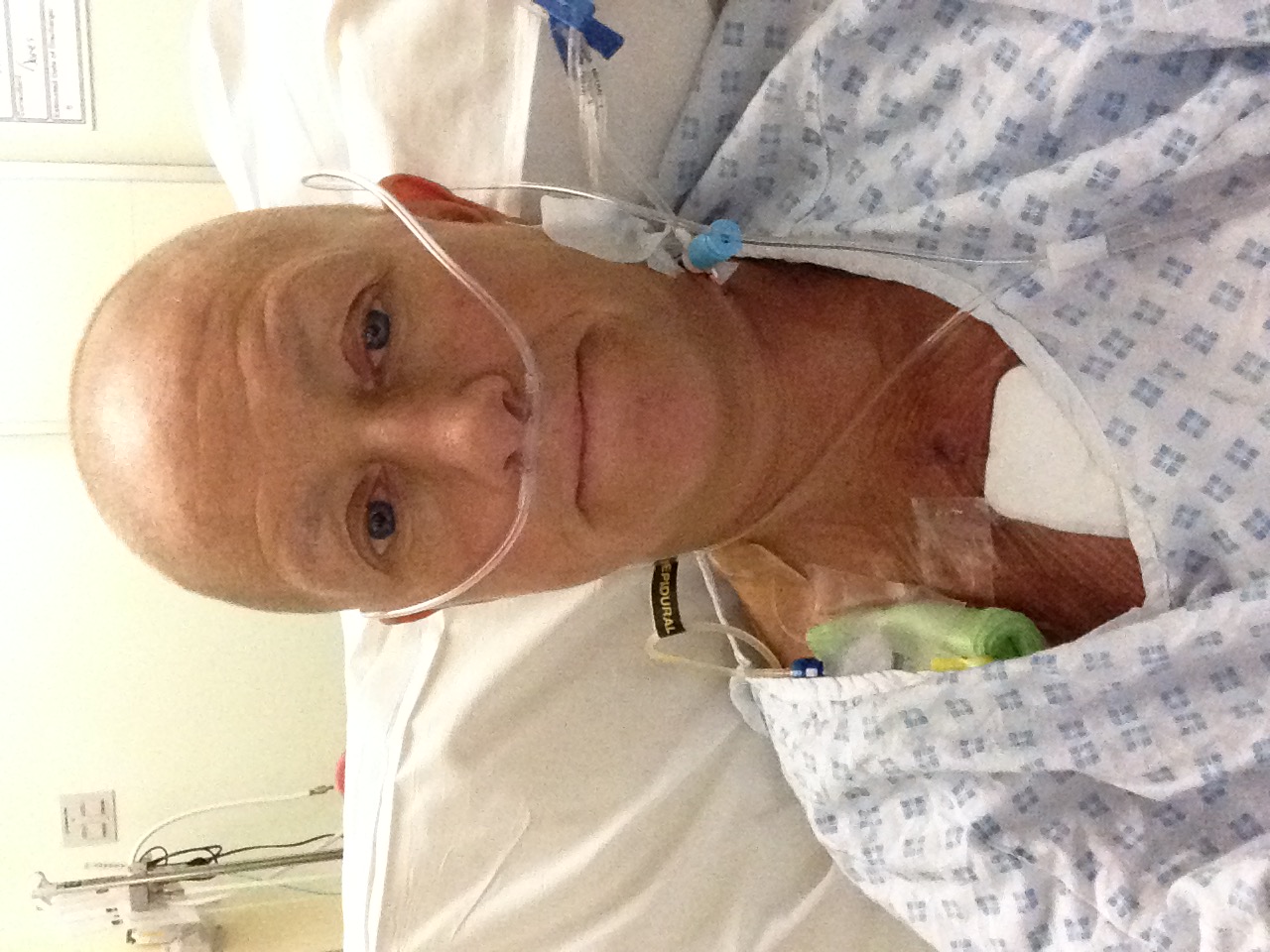
I was wheeled in the bed up to the unit and tubes coming out from everywhere. They moved me into the bed and then sorted all the wires out and attachments and even only just come out of OR I was worried about someone catching one of the wires and surely enough one of the recovery nurses who was learning the drill caught my two central lines stitched into my neck which proceeded me to “go with it” and go “aghhhhh!” lifting my upper body out of the bed (not really good when you’ve just had your sternum removed) anyway, still intact I was finally settled.
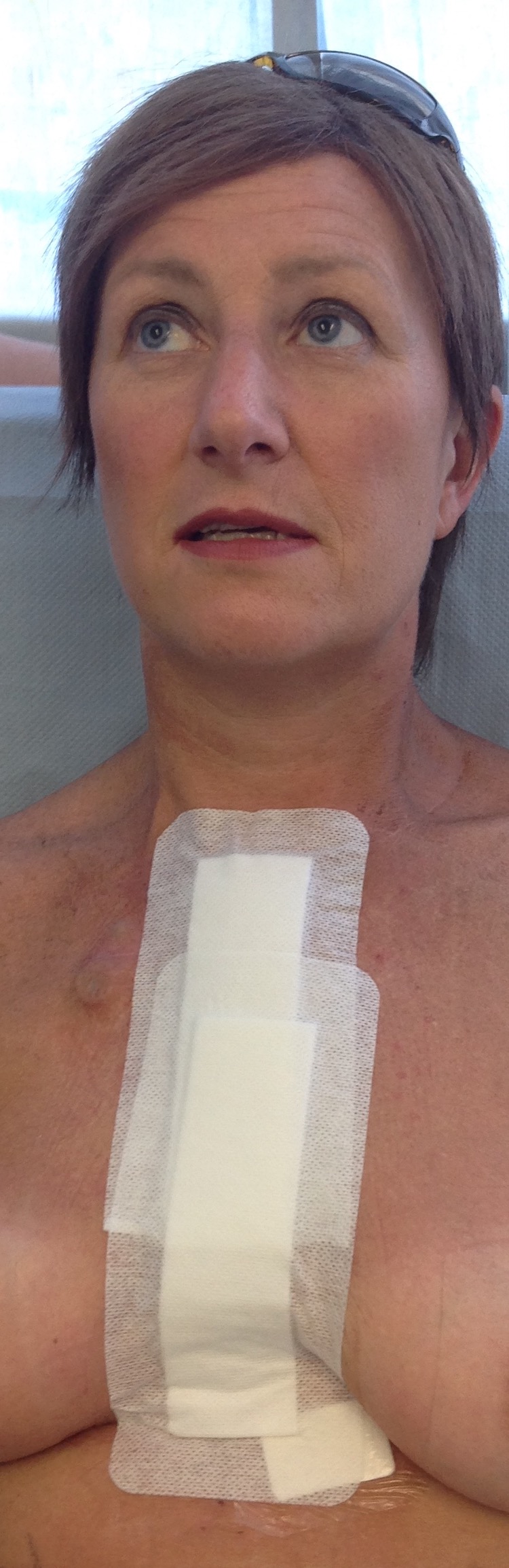
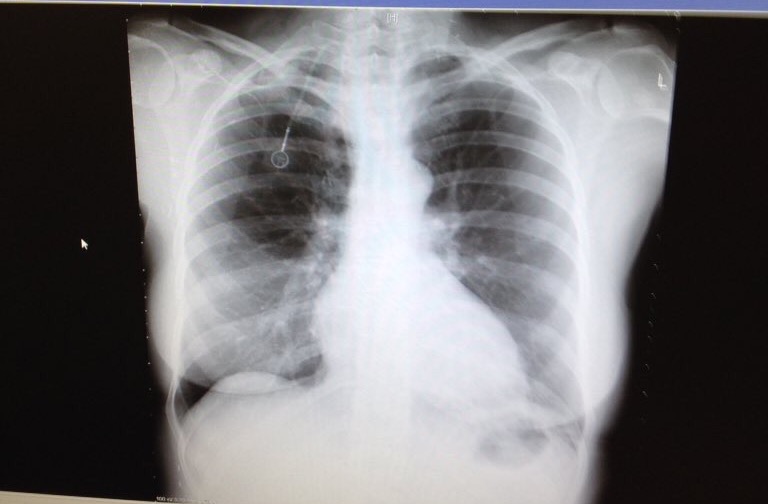
So to give you the picture of what was happening in Critical Care Unit, I had a nurse who was dedicated to me and one other patient. I had an IV in a central line in left neck in jugular vein so I can have antibiotics or adrenaline, two lines in my left wrist. 3 drains in my mid chest area – one in each lung and one for the sternum area, an epidural in my back giving a pain block for pain relief. Self-administering alternative to morphine so less SEs but ended up on anti-sickness as still feel sick. Pain in recon boob & stingy feeling in sternum (even though numb). I had a PICO dressing on my sternum which was a vacuum battery operated small pump to stop any oedema or swelling to the area, ECG monitor, Catheter, DVT injections daily, compression socks & anti DVT blow up things on my legs which blow up alternate leg every damn minute… BUT apart from that I felt OK! Surgery went well & I had not lost my right reconstruction implant or had to have it removed. The Oncoplastic surgeon basically pushed it out of the way to get to the pectoral muscles which had been lifted and crossed over my mid sternum line.
I had a saline drip as dehydrated still from op but around 6pm had to ask for tea and toast as was starving and very thirsty so drunk 4 teas & 5 glasses of water. The toast took ages to swallow and when Jeff came to see me I asked him to bring strawberries and blueberries as I knew my mouth would feel horrible. When he left I tried sleeping but kept being woken up every minute by the leg DVT pumpers I asked for them to be turned off and I got off to sleep around 1am then woke around 2am, only to start heaving and sat in bed trying not to heave as I was worried about my sternum and causing a problem, I sat and was sick after the fruit I had eaten…
I drifted off around 3am for a couple of hours. I recovered my phone and iPad around 10pm the previous night as my bag was “lost in transit” from the OR. Next day I was able to get back to some of the lovely messages. I was unable to get up out of bed and until the epidural was removed therefore I had to keep the catheter in.
5am and the nurse just helped me get comfy again as woke up shivering in pain, I was much comfier after more painkillers and then brushed my teeth in bed. The nurses were wonderful and the one on nights that night R was a darling, so caring, and swore she knew me and we found out that she may have cared for me in The Christie 9 years ago when I was admitted due to issues with chemo.
Two days in and l was still on the CCU had a bad day yesterday as sat in a very uncomfy chair from 7.30 am till 6pm when I asked to go to bed. I had a few really low BP issues, dizzy and was completely spaced out when they gave me a high dose morphine, adrenaline and other drugs, couldn’t feel fingers and bang I was back. Phew, not a nice feeling.. I wasn’t walking, only standing with help from chair to bed. So the next day I had 2 drains out from my lungs – that was pretty yuk – you can’t fill your lungs enough with air and they ask you to breathe in and if you can’t do it enough it may mean you get fluid on your lungs so we did 3 practice breaths before I felt ok about them doing this. A shot of morphine ½ hour before and they were out. I still had the mid line drain in, epidural and PICO dressing. Epidural was due to be removed the next day ugh. They were going to take out the central line too from my neck so I wasn’t looking forward to that.
I was given a lung volume measurement device to measure your lung capacity you have when you fill your lungs. Sore or not you had to do exercises every day with arms up, sucking into the device (recording 1000 first time – ‘normal’ lung capacity was around 3000!) and then holding a towel on my chest and coughing and pushing air out of my lungs with my mouth in an O shape. It was hard not to be scared doing these things knowing the operation I had. It also cleared the chest so you didn’t have any problems with fluid going onto them. Every time a surgeon did the rounds you were asked to cough and they checked the fluid.
The nurses who cared for me were so kind and considerate, every day I was washed and a new clean gown and I could brush my teeth in a bowl and helped to be comfortable. Unfortunately (or fortunately) I was unable to move to the other ward for 3 days due to bed availability. I didn’t actually mind as it was great to have such amazing care. They also moved the bed to the back of the area and then sat you in a chair (it was basically a shuffle for 2 days) to get you up and out of bed. Every time was like a military operation with two nurses so I didn’t fall or drip over my many tubes. It’s shocking how weak you are and then as the days went on and more and more tubes were disconnected and lines taken out you get feeling stronger. The third day I had a chat with a chap who was another Physio on the ward and he was asking me all about what I did and what op etc and he said – right so do you want to go for a walk then? My nurse who was caring for me looked over and I said is it ok? She agreed and they both took me for a walk around the ward block! He said I did really well and I was pleased I could do it, wobbly but I could do it again.
The Thursday I mentioned to the surgeon who came to see me every day that I had to hold onto the back of my head when lifting my head off the pillow and she said “ah yes we’ve also had to detach your neck muscles that run down the front of your neck and reattached them to the clavicle area” OUCH – no wonder I felt so crap and in pain there. Ah well…
So Friday I was able to get the epidural and catheter out and the central line was removed and had to lie down for 1\2 hour after this procedure otherwise my vein would be spurting blood out of the jugular! The IV in the hand had come out the previous day as it had stopped working. Excellent care but poor food. I had lots of visitors and thanks to all who came into see me. The lady who had this op done before me, whom I had met, came into see me Thursday night which was lovely, she brought a survival pack of muesli, banana, strawberries and blueberries, some gorgous nutty bread and a yoghurt. Two friends from WoMMeN project team Dr L and Dr J also came to see me, so that was lovely and then on the Friday another friend from the WoMMeN project and two other friends. Other friends came to see me too which was great support.
I finally got to F6 ward where there was only 4 beds and I was met with one of the ladies who was having her “stomach measured” as she obviously had issues from the chat which was ongoing but it was the funniest thing and her and the HCA were having the most outrageous banter with each other to the point where I had to hold my towel on my chest as I was laughing that much…
Nurse “look its 16 centimetres!”
Patient “no it’s not, it’s more than that, bloody give it here – oh I’m going back to bed!”
Nurse “I don’t know how to do it! Get up out of bed!”
Cue another nurse came along to try to help measure and the madness still ensued with this stubborn patient and the nurse.
I was howling and I just knew I’d have a bit of fun.
L was totally outrageous sometimes and had lots of ‘life knowledge’ one minute she would have me laughing the next telling me such a story it made me want to cry. In 2 days we knew quiet a lot about each other and the other lady in the room S. There was another lady who seemed really poorly and slept most of the Saturday. S was like my mum and very strong willed and found out she used to be a national fencing champion. L as I said had so many life experiences but could tell even though she left school at 15 she was very well read, educated and very intelligent and knowledgeable. All 3 ladies were in due to having heart attacks. The symptoms were all missed and they didn’t have a clue that just indigestion could mean that they were having a heart attack. All 3 had had bypasses and two had been in 4 weeks! So they were amazed when I was going home 5 days after my op! Toilet talk was the highlight of the day with L and myself, who’s been and who’s not and what to do about it next as I handed over a bag of prunes and apricots to L and she wolfed them. I hope they worked!
The threat of an enema for me was enough to get things moving finally after 8 lots of laxatives, suppositories etc… YAY!
The nicest thing L said to me was that I was a really calm person (I am without 2 kids!) and I obviously knew what I was doing, and why, and she was amazed at how I’d handled all of this. I really bonded with her and loved her sense of humor and vulnerability. Anyway, I was able to come home the Sunday and said goodbye to them and I hope they are all keeping well.
So I’m glad I’ve had it done but could not drive for at least 5 weeks or do any exercises that will put strain on the pectoral muscles I’ve had moved otherwise they will rip (yes the surgeon was that specific).
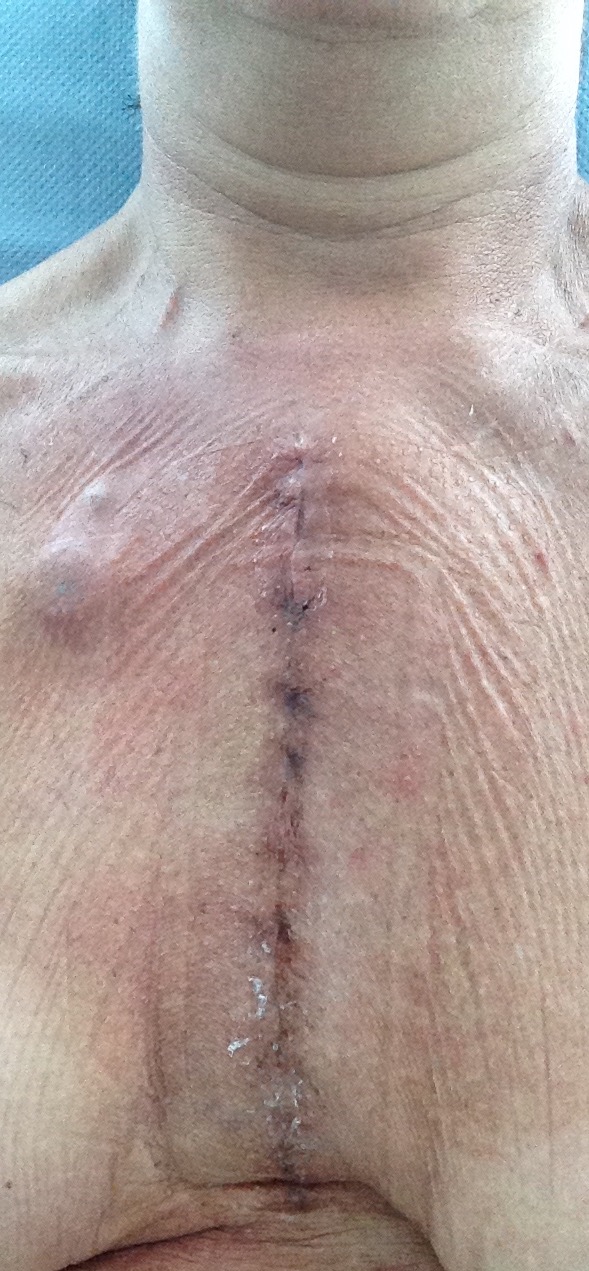
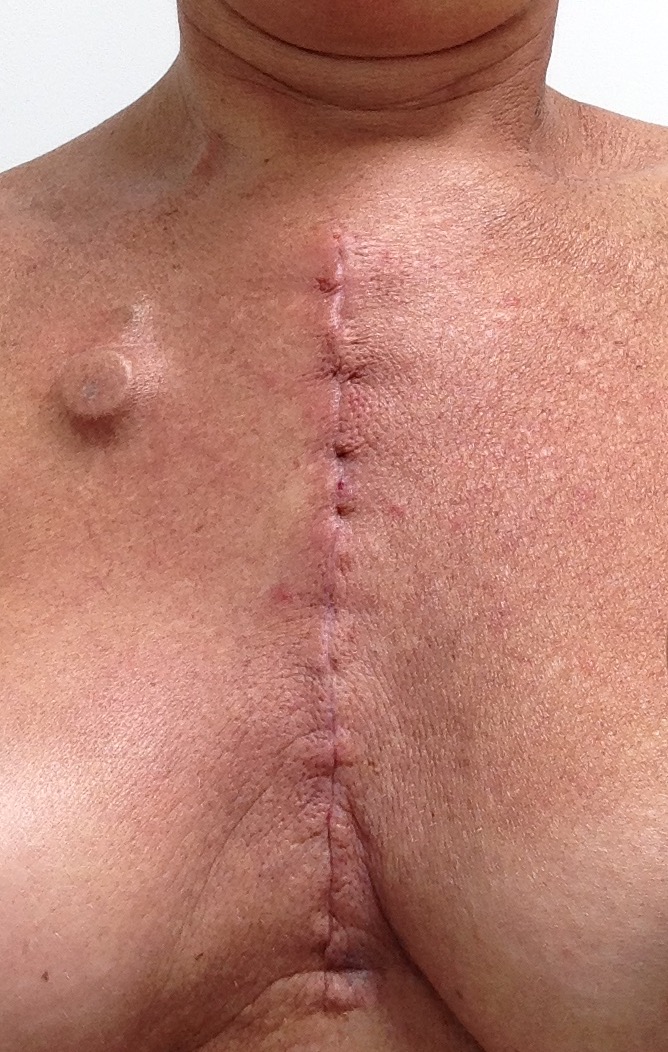
To give you the lowdown on exactly what surgery I had done, the cardio thoracic surgeons (2) removed my top two parts of the sternum at the top, left the bottom bit in place which gives rigidity to the whole thing and there are around 6 ribs that come off this part too. Then replaced the sternum area with a composite material and cemented the area for stability. They then reattach the ribs they had detached back onto the new sternum. The Oncoplastic surgeon then used my pectoral muscles and pulled them across (crossed over) to basically shield the area with some solid flesh so that it was held in place.
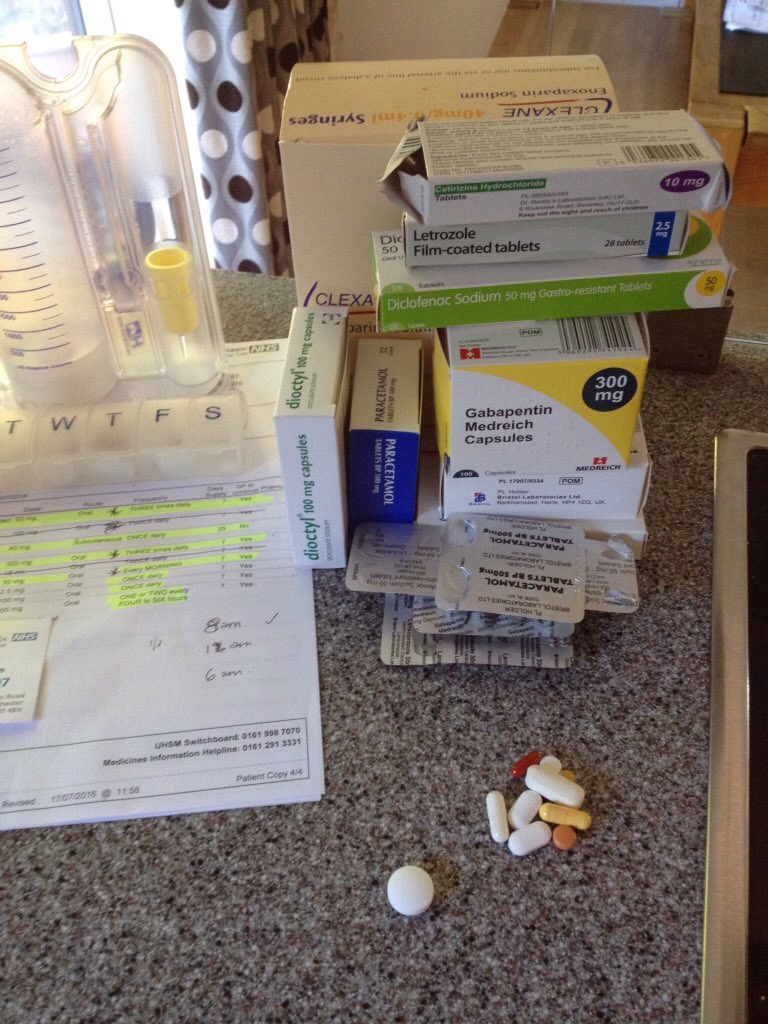
So back home and thrown the next day into looking after the kids as school holidays started that Monday for Faron and Regan finished on the Wednesday. No rest for the wicked eh? I’ve been sleeping on a wedge of pillows sat in an upright position as it’s uncomfortable to sleep lie down and no way can I lie on my side. I wonder if I’ll ever be able to lie in my favourite position on my front… Everything crunches when I move or lie on my side and I’m still using my hand to pull myself out of bed behind my neck. I kind of use a wheel motion, hold the back of my head with one hand and then behind my knee with the other and roll like a wheel in bed to get up, or just try to somehow pull myself up. Seriously sometimes I feel bloody 90 and drag my sorry self up and out of bed. Nothing is comfy anymore and I’m hoping it will pass. Soon. Please. I was taking nerve painkillers but stopped the strong painkillers before I came out of hospital. So was on a type of strong ibuprofen, nerve pain killers, paracetamol and a few other bits and pieces and then having Clexane blood thinning injections for 25 days. I also was told to wear the DVT socks for SIX WEEKS (thank goodness were not having a summer!)
So 9 days after this I attended the Breast Cancer Now Research Symposium in London – yes I know it was a mad thing to do but seriously I was OK and I wouldn’t have put myself into any danger and put my operation at risk. Have a look at the link here: https://www.facebook.com/abcdiagnosis/posts/971176729644209
Three weeks in was the most pain and discomfort that I had. I felt in a big block of pain on my chest. The issues I have are also from 9 years ago and I still have pain in my right breast after the LD reconstruction from 9 years ago, my back is still sore and have nerve damage there. Then a year ago I had a full removal of all left neck nodes (13 stitches – unlucky for some) and radiotherapy causing numbness around there and my shoulder. Then left shoulder mets with radiotherapy back and front causing pain and numbness there. Now my sternum removed and the surgery as detailed above. My arms are weak – it’s shocking how much you use your chest muscles in daily life. Even when I was in hospital I would go to the toilet and I found it so hard to use a press flush toilet as the action was really difficult to press it due to those muscles. Opening cans is another thing, really difficult. And getting up and out of bed is seriously causing me lots of pain and last week when I lay down flat I was getting lots of back pain so reverted back to the sitting up position. And then I’ve had problems bending and getting socks and shoes on so thankfully my little angel Faron has been at hand to help her Mummy.
It’s been hard not being able to get out in the car with the kids for 5 weeks since out of hospital. But got the go ahead after my appointment with Mr O at Wythenshawe 5 weeks after surgery. I also needed to see him due to pain in my neck I had been having but he was very, very pleased and amazed at my recovery. Neck pain is normal after detachment of the muscles. Surprised I could even take my top off and get my arms somewhat behind my back over my head. I told him how stiff I was and he did say it is early days and showed Jeff how to press on my shoulders to push them back but gently as still a risk of stitches to rip if too heavy. He had a look at the scar and told me it looked good. The back and shoulder pain is obviously all related. But good news is that I can go back to running! Sadly not allowed to cycle for another few weeks as they need to know that everything has knitted together before letting me out on the bike so that means I can’t do the 100 Mile Manchester charity bike ride I had planned to do for The Christie on 4th September. So waiting for the biopsy results but they won’t be ready for another couple of weeks so fingers crossed for the same biology as I’ve had before.
Another positive is my CA15-3 tumour markers are down again so obviously something is working (down to chemo I guess) and hopefully now I’ve had the sternum removed then another source of cancer growth will have been eliminated.
Annoyingly I will have to have another 3 cycles of chemo starting 30th August after the planned abcd exercise retreat – had to defer treatment a week otherwise I would have been ill and unable to organize the retreat which would have been a disaster. I totally understand why have to have chemo and I guess I’ve made peace with that but definitely going to have the cold cap – I can’t face losing my hair for a 4th time…
After all this I know I’m never going to be the same and every op I’ve had cuts further into my life a little more. I just hope it’s worth it for a remission – if not I’ve given up quality of life for what? I’m living in hope again.
P.S. Thank you again so much to the amazing staff at University Hospital South Manchester for looking after me especially to Kate, Emma, Sarah, Sophie, Cini, Ruth, Mr J, Mr O, Mrs O’C, Fedro, Tony, the dressings dept, secretaries and the many staff that helped me in the Critical Care Unit and the staff on F6 ward, I wont forget your understanding and kindness.